My colleagues and I are on our way home from the first delivery of a specialized newborn care course delivered to nurses, midwives and clinicians in Central Malawi. The Specialized Newborn Care Education (SNCE) is a capacity building component of the Canada-Africa Initiative to Address Maternal, Newborn and Child Mortality (CAIA-MNCM), funded by the Government of Canada through Global Affairs Canada. The SickKids Centre for Global Child Health is partnering with Amref Health Africa in Canada and health systems partners in Malawi to provide capacity building support by developing and delivering this education. The SNCE will be delivered in Malawi, Ethiopia and Tanzania over the next four years to 45 health workers in each country.
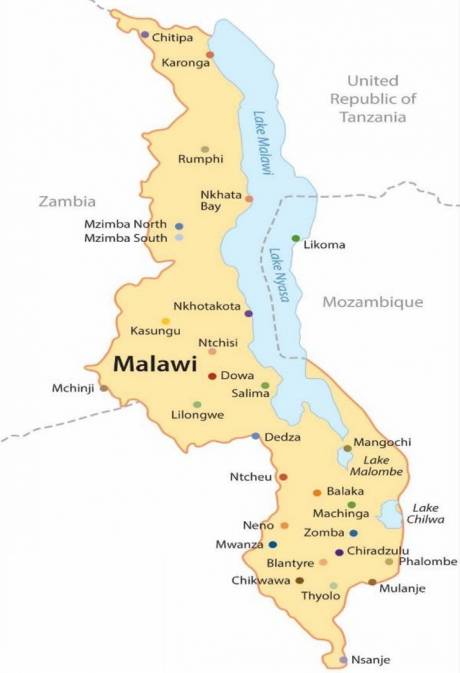
Ntchisi, Malawi, the site of the first delivery, is located just north of the Malawian capital of Lilongwe and has a population of about 200,000 and was a priority for training because of the high rate of newborn deaths compared to other districts in Malawi. Ntchisi District Hospital is a busy district facility that takes referrals from the 10 surrounding health centres. Driving to and from the hospital each day, we could appreciate the distance families have to travel over difficult terrain to receive health care in this rural landscape.

We were very fortunate to work with a diverse team of Malawian colleagues to support the training. Local Ministry of Health partners and Amref Health Africa in Malawi were engaged to co-facilitate the SNCE, and provided invaluable local context and expertise. Dr. Shiphrah Kuria, Reproductive Health & Family Planning Program Manager from Amref Health Africa Headquarters, also joined us from Nairobi to co-facilitate. She helped empower the students to provide excellence in clinical care through her passionate commitment to maternal and newborn health. Together, we were a powerful and enthusiastic team with a deep desire to inspire local health workers to provide high quality care to newborns.

Teaching in the clinical setting was invaluable to integrate the learnings in the classroom into clinical practice. Facilitators provided guidance and mentorship around evidence-informed practices while adjusting care to the reality of the daily clinical challenges that arise from things like accessing clean water, medication stock-outs and staff shortages.
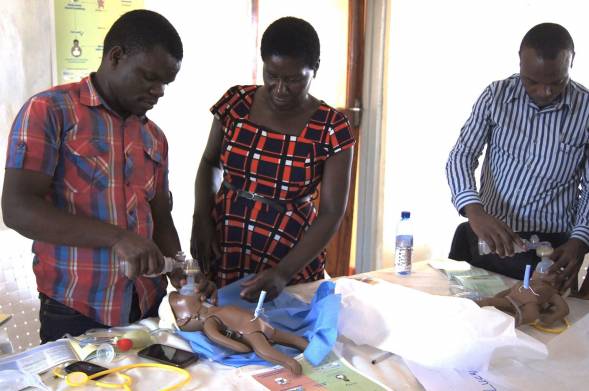
Malawi has made significant strides in newborn care over the past decade. Our goal was to highlight the successes while recognizing the gaps in care that could have a significant impact on outcomes, often with simple, yet effective, solutions. The SNCE was designed to be interactive, hands-on learning that reinforces best practice guidelines and focuses on the three major causes of neonatal death: birth asphyxia, infections and preterm birth. To facilitate the classroom learning we used simulator baby models to practice implementing guidelines and master key clinical skills. This kept the learning fun and active!
Breastfeeding Education
 One very memorable section of the course was the teaching of manual expression of breast milk using the MamaBreast simulators. MamaBreasts allow participants, male or female, to appreciate just how difficult and time consuming it is for mothers to express breast milk! The breasts are filled with water and only ‘express’ when the technique is followed perfectly. This provided a great opportunity for health workers to practice educating their peers, who act as new mothers, in this challenging task. It also provided lots of laughs as participants struggled to express even a tablespoon of liquid from the MamaBreast simulator.
One very memorable section of the course was the teaching of manual expression of breast milk using the MamaBreast simulators. MamaBreasts allow participants, male or female, to appreciate just how difficult and time consuming it is for mothers to express breast milk! The breasts are filled with water and only ‘express’ when the technique is followed perfectly. This provided a great opportunity for health workers to practice educating their peers, who act as new mothers, in this challenging task. It also provided lots of laughs as participants struggled to express even a tablespoon of liquid from the MamaBreast simulator.
Treating Respiratory Distress
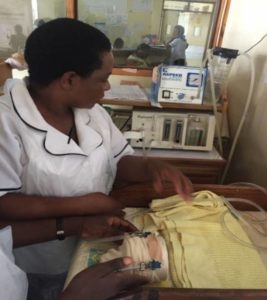 Malawi has been at the forefront of trialing a device, known as bubble Continuous Positive Airway Pressure (bCPAP) machine, used to treat respiratory distress in newborns. For learning, we crafted a ‘baby’ out of a roll of dressing gauze to practice setting-up and using the bCPAP. We then had the opportunity to use the device on newborns in the hospital who were in respiratory distress. The groups’ confidence with the technology and understanding of its benefits increased immensely, which we hope will lead to more widespread use in the Ntchisi nursery.
Malawi has been at the forefront of trialing a device, known as bubble Continuous Positive Airway Pressure (bCPAP) machine, used to treat respiratory distress in newborns. For learning, we crafted a ‘baby’ out of a roll of dressing gauze to practice setting-up and using the bCPAP. We then had the opportunity to use the device on newborns in the hospital who were in respiratory distress. The groups’ confidence with the technology and understanding of its benefits increased immensely, which we hope will lead to more widespread use in the Ntchisi nursery.
Identifying and Preventing Early Infection

According to the WHO, newborn infection is the leading cause of neonatal death worldwide, comprising a staggering 45% of all neonatal deaths (World Health Statistics, 2016). Preventing infection was a major theme throughout the training with an ongoing focus on hand washing as the simplest, most effective means of infection prevention and control. To reinforce this, we used a GloGerm activity that shines an ultraviolet light on washed hands to show areas that are frequently missed such as the nail beds and between the fingers. It served as a fun way to reinforce a simple, inexpensive way to prevent infection that can truly save the lives of newborns at risk.
Agents of Change
 Leadership was a focus throughout the training. Our goal was to empower health workers to lead sustainable changes in their daily clinical practice and to strengthen their role as clinical leaders by focusing on communication, self-reflection, the power of educating families and providing respectful, compassionate care. At the close of the training, each participant was challenged with the task of becoming an “Agent of Change” by identifying a specific, realistic change/goal to implement in their own clinical area. One participant committed to measuring every newborn’s temperature to ensure babies are kept warm and close to their mothers after birth. Another plans to ensure each baby is weighed at their one-week follow-up visit to ensure weight gain is tracked. Each is an example of a step towards improving newborn care using simple, potentially life-saving interventions.
Leadership was a focus throughout the training. Our goal was to empower health workers to lead sustainable changes in their daily clinical practice and to strengthen their role as clinical leaders by focusing on communication, self-reflection, the power of educating families and providing respectful, compassionate care. At the close of the training, each participant was challenged with the task of becoming an “Agent of Change” by identifying a specific, realistic change/goal to implement in their own clinical area. One participant committed to measuring every newborn’s temperature to ensure babies are kept warm and close to their mothers after birth. Another plans to ensure each baby is weighed at their one-week follow-up visit to ensure weight gain is tracked. Each is an example of a step towards improving newborn care using simple, potentially life-saving interventions.
Counting Every Newborn Life by Making Health Workers Count
 Each participant left the training with a renewed sense of urgency to improve newborn care. As facilitators, we felt inspired by their energy and passion for their country and the future of their health system. Through collaboration with partners like Amref Health Africa, measurable, key changes are being made, one clinician at a time. By making each newborn count, health workers strive to provide the best care possible to each and every family.
Each participant left the training with a renewed sense of urgency to improve newborn care. As facilitators, we felt inspired by their energy and passion for their country and the future of their health system. Through collaboration with partners like Amref Health Africa, measurable, key changes are being made, one clinician at a time. By making each newborn count, health workers strive to provide the best care possible to each and every family.
About The Canada-Africa Initiative to Address Maternal, Newborn and Child Mortality